13 Feb Serious Considerations Regarding Colonoscopies

Paul A. Goldberg, MPH,DC,DACBN,DCBCN
As a Professor of Public Health and as a Clinician I have concerns about a number of common practices within the arena of so called Preventive Medicine. Preventing disease as opposed to waiting for organic problems to occur is wise. The manner in which “Prevention” has often been employed in Preventive Medicine, however, has led to injuries and fatalities that would otherwise not have occurred, violating the Hippocratic Dictum of “above all do no harm”.
Perhaps the worst offenders in the Preventive Medicine realm are yearly mammograms that expose patients to cancer inducing radiation and the routine use of colonoscopies to be addressed herein.
It is estimated that 51,020 deaths will be attributed to colorectal cancer this year as the second leading cause of cancer death in the United States [1]. This has generated the widespread use of colonoscopies.
 Colonoscopies employ a camera inserted into the colon called a “colonoscope.” These have become routine procedures in Medicine for the identification of cancer or precancerous tissues/polyps. As the physician guides the colonoscope through the colon biopsies are taken of suspicious tissues.
Colonoscopies employ a camera inserted into the colon called a “colonoscope.” These have become routine procedures in Medicine for the identification of cancer or precancerous tissues/polyps. As the physician guides the colonoscope through the colon biopsies are taken of suspicious tissues.
Colonoscopies are performed about 50,000 times per day in the U.S. in hospitals and clinics or about nineteen million per year [2]. Most are labeled as preventive or as routine screenings. The more red flags on a patient’s health history e.g. having a family history of colon cancer, inflammatory bowel disease or other factors associated with the genesis of cancer, the more frequently they are performed sometimes as often as twice per year.
The rationale of preventing cancer is appealing but there are questions to be considered regarding routine colonoscopies in light of their potential complications.
The three most common complications are[3]:
- Adverse reaction to the sedative used during the exam
- Bleeding from the site of biopsy or where abnormal tissue was removed
- A tear in the colon or rectum wall (perforation)
Colonic perforation is the most serious of these and may result from mechanical forces against the bowel wall, barotrauma, or electrocautery. It is associated with a high rate of morbidity and mortality. [4]
The rate of colonic perforation, based on statistics from Baylor University Medical Center, is about 1 out of every 1,750 procedures performed. Based on nineteen million plus procedures per year, a total of almost 11,000 perforated colons result from colonoscopy annually.[5]
If you are one of those 11,000 individuals that suffers from a bowel perforation the assurance that bowel perforation rates are low is no comfort.
There are two additional concerns regarding colonoscopies.
A little talked about issue that occurs with every person undergoing colonoscopy is that of bacterial translocation. There are different types of bacteria that reside in different areas of the colon. Some species are prevalent in the ascending colon, some in the transverse colon, others in the descending colon. These bacteria have different properties and are intended to reside in specific areas of the large intestine to perform specific tasks. When the colonoscope is inserted it transports bacteria from the lower part of the colon to the middle and upper portions. When it is withdrawn it carries bacteria native to the upper portion of the bowel to the lower end. This can greatly disturb the microbial balance of the microbiome and lead to significant functional issues, which later can manifest as organic disease.
The other issue is the introduction of colonoscopes into the patient’s colon that are contaminated from prior usage. This can result in great mischief including transmission of a number of diseases. Instances of patients being infected with bacteria laden colonoscopes have been well documented.
The recent video (shown below) of our patient Ms. Linda Good documents the potential misery and long term complications that can result from routine colonoscopies.
The colonoscope utilized with Ms. Good had not been properly sterilized and she contracted Clostridium Difficile as a result, was hospitalized and administered antibiotics. She developed Ulcerative Colitis from the Clostridium Difficile and was placed on steroids. The steroids led to immune system suppression and the development of Clostridium Difficile two additional times. Ms. Good continued to have Ulcerative Colitis symptoms and was given a plethora of drugs including entocort, lialda, sulphasalazine and asacol over the next ten years. She was also given herbs and supplements from a “functional” doctor while her condition continued to deteriorate.
In 2019, Ms. Good’s joints became swollen and painful. She consulted with a Rheumatologist who diagnosed her with Lupus and administered steroids, imuran, cymbalta and muscle relaxers. The steroids put her into a diabetic range and caused her to develop mood swings, gain weight and experience hair loss. Her Medical Physician told her she would be on drugs for life and couldn’t survive without them.
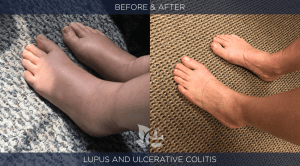
After consulting with us and being put through an individualized Bio-Hygienic Re-Creation Program™ Ms. Good is now entirely recovered and drug free. See before / after pictures below. Click here to see Linda’s before / after lab studies.
 .
. 
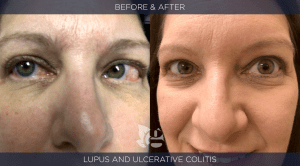
Ms. Good related that as she was being put under for the colonoscopy she heard a nurse comment that they “could not locate the colonoscope selected initially but here is another one we can use”. A decade of illness and suffering for a “Preventive” Measure.”
The use of disposable colonoscopes developed in Israel are prudent to consider in this regard but their use is not common at this time.
The fear of rectal and bowel cancer is understandable. Colonoscopies can identify precancerous tissues and in some cases their removal might extend the person’s life even though the causes of cancer that formed that abnormal growth remain.
There are factors that have been identified in cancer causation; inter-related lifestyle, nutritional, biochemical and microbiological factors that can then be addressed without risk to the patient. This can greatly enhance a patient’s health and their resistance to cancer without risk to the patient.
None of this is to imply that colonoscopies should never be performed. There are cases where one might be indicated. We should, however, be prudent in making a decision to undergo routine colonoscopy and understand the risks involved.
[1] https://www.cancer.net/cancer-types/colorectal-cancer/statistics
[2] https://idataresearch.com/an-astounding-19-million-colonoscopies-are-performed-annually-in-the-united-states/
[3] https://www.mayoclinic.org/tests-procedures/colonoscopy/about/pac-20393569
[4] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2811793/
[5] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4264696/




AffiliateLabz
Posted at 22:33h, 15 FebruaryGreat content! Super high-quality! Keep it up! :)
David Tener
Posted at 02:52h, 23 FebruaryThank you! Glad to hear the information is of value to you.
Ray petty
Posted at 19:33h, 19 FebruaryThanks for article. I hope to visit your clinic someday.
David Tener
Posted at 02:45h, 23 FebruaryThank you, Mr. Petty. We will be glad to assist you.
Ray petty
Posted at 21:25h, 19 FebruaryIsn’t a colonoscopy needed if you suspect a patient of having UC but they haven’t been diagnosed yet? Thanks
David Tener
Posted at 02:51h, 23 FebruaryThe article is not to imply that colonoscopies should never be performed. There are situations where one might be needed and this should be determined on a case by case basis.
I recommend reading our two part article on Inflammatory Bowel Disease which discusses our approach to this increasingly common health problem in detail. Part I: https://www.goldbergtenerclinic.com/blog/tackling-inflammatory-bowel-disease/. Part II: https://www.goldbergtenerclinic.com/blog/tackling-inflammatory-bowel-disease-part-ii/.
Donald Portland
Posted at 12:32h, 10 MarchIt¡¦s in point of fact a great and helpful piece of info. I am glad that you simply shared this helpful information with us. Please stay us up to date like this. Thanks for sharing.
David Tener
Posted at 13:03h, 10 MarchThank you Mr. Portland. We appreciate your feedback and are glad you found the article of value.
Chris StLuise
Posted at 18:28h, 11 AprilGreat article ! People never hear the other side of this story and think they can eat haphazardly and the surgery will bail them out if a problem shows up.