02 Feb Blood Sugar: Beyond Diabetes and Hypoglycemia (Part I)

 Paul A. Goldberg MPH, DC, DACBN, DCBCN
Paul A. Goldberg MPH, DC, DACBN, DCBCN
Consultant to The Goldberg Tener Clinic
Chronic Disease Reversal
Click here to read Part II of this article.
As a Clinician and Professor of Clinical Nutrition working to reverse chronic illnesses with patients for almost fifty years, I’ve been involved both clinically and academically with blood glucose physiology, biochemistry and clinical applications of blood glucose regulation in a wide variety of health issues. I continue to appreciate the enormous complexity of how the body regulates its energy supply and the numerous clinical ramifications that occur when it becomes compromised.
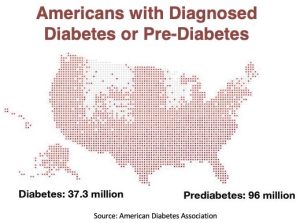 Most people, whether a layperson or healthcare professional, consider blood sugar issues to basically revolve around diabetes (insulin dependent, non-insulin dependent or gestational diabetes where blood glucose levels are excessive), hypoglycemia (low blood sugar), dysglycemia ( referring to high and/or low blood glucose) or pre-diabetes. These categories alone affect over forty percent of the Adult U.S. Population, yet even with this large percent of the population affected there is more to the story of how blood sugar issues affect chronically ill people whether they have received one of these diagnoses or not.
Most people, whether a layperson or healthcare professional, consider blood sugar issues to basically revolve around diabetes (insulin dependent, non-insulin dependent or gestational diabetes where blood glucose levels are excessive), hypoglycemia (low blood sugar), dysglycemia ( referring to high and/or low blood glucose) or pre-diabetes. These categories alone affect over forty percent of the Adult U.S. Population, yet even with this large percent of the population affected there is more to the story of how blood sugar issues affect chronically ill people whether they have received one of these diagnoses or not.
A large percentage of patients we work with in reversing chronic disease have impaired blood glucose regulation regardless of their medical diagnosis including many who have not been medically diagnosed with diabetes or pre-diabetes of any sort. This includes many patients with autoimmune illness (one hundred plus different diagnoses), cardiovascular disease, premature aging, senility, digestive issues including Irritable Bowel Syndrome and Inflammatory Bowel Disease, chronic fatigue, depression, learning disorders, infertility, poor libido, vision issues, sleep disorders, osteoarthritis, skin issues, environmental allergies, drug/alcohol addictions, obesity and anxiety. These and many other disease issues frequently have blood sugar regulatory issues behind them that are not uncovered medically and has compromised our patient’s ability to regain their health.
How could so many people have un-addressed glucose dysregulation behind their health problems?
Blood glucose regulation is complex. It is not simply a matter of your insulin output or your insulin resistance. It is not just a dietary issue. It cannot be discounted simply because someone has a normal fasting glucose or HgA1C .
Keeping stable blood glucose levels is a body priority just as is respiration. All body systems are affected by glucose levels and likewise virtually the entire body plays a role in its regulation. This includes not only the pancreatic Islets of Langerhans which produce insulin but also glucagon from the alpha cells of the pancreas and hormones from the pituitary, thyroid and adrenal glands e.g., TSH, Thyroxin, Cortisol and adrenalin. The liver plays a major role in blood sugar control storing glycogen, the storage form of glucose, and releasing it as needed when the blood sugar levels fall. There are specialized intestinal cells producing sugar and fat splitting enzymes e.g., maltase, lactase, sucrase, lipase. The gastrointestinal tract, circulatory system and nervous system all play important roles in blood glucose regulation.
Blood sugar is required for the operation of most cells in the body or when not available, the production of ketone bodies is essential to act as an alternative fuel source. The nervous system including the brain, spinal cord and peripheral nervous system, all require a steady supply of glucose. Glucose is mostly derived from dietary carbohydrates although it can be formed from protein as well if necessary. When glucose is not available, a diverse assortment of symptoms can present themselves, many not associated by practitioners or laypersons with blood sugar impairment. Physical symptoms of disease, including chronic inflammation, are produced in a wide range of circumstances when glucose regulation mechanisms are impaired. It is indeed essential in reversing most chronic inflammatory conditions that blood sugar regulating mechanisms be addressed and corrected.
Assessment of Blood Glucose Regulation
A thorough case history remains the priority in assessing Glucose Regulating Issues as with other health problems. This generally requires a full hour with the doctor, followed by a physical examination and comprehensive laboratory evaluation. Questionnaires focusing on symptoms such as fatigue, digestive efficiency, depression/anxiety, sleep patterns, lack of mental acuity, food cravings, joint and muscle discomforts, dietary intake patterns, signs of premature aging, etc. are also useful.
Primary lab evaluations geared towards blood glucose assessment include fasting glucose, hemoglobin A1C (HgA1C), Fasting Insulin level and importantly (but infrequently performed by most clinics due to its complexity), the 5–6-hour glucose tolerance test.
The Glucose Tolerance Test
No single test can completely evaluate glucose regulation. The Glucose Tolerance Test (GTT) when administered and interpreted correctly, however, in combination with the HgA1C, gives us an excellent source to identify and address issues from. The GTT looks at the body’s ability to handle and balance glucose under physiological stress.
We would not evaluate a car simply by starting it and listening to it idle. We must put the car through its paces… go uphill, accelerate and see how the car performs under real life driving conditions. The same can be said for the Glucose Tolerance Test. It is not merely a test of what the blood sugar is when the body is at rest but a test of how the entire body works to control blood sugar when put under physiological stress over a prescribed time period.
It is a lengthier, more complex and time-consuming test to run and requires significant clinical experience to be properly interpreted. Being more time and labor intensive, it is not commonly performed by clinicians compared to other studies. As such, most physicians lack the skill in administering it properly, interpreting it fully and making sound application of it.
One major error we commonly see is that the GTT is ordered for too short a period of time, i.e., three hours or less when it should be done preferably for five or six hours. A two-hour GTT test as it is often performed greatly undercuts its value and will miss important clinical information. While a two-hour test may identify full blown diabetes mellitus it will entirely miss identifying hypoglycemia, dysglycemia as well as numerous individual variations that can provide valuable information needed to address and improve the patient’s metabolic issues.
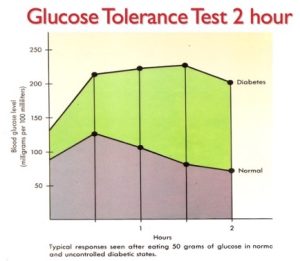
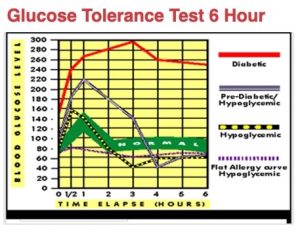
Performing the Glucose Tolerance Test
The patient arrives at the lab in a fasting state in the morning. Their fasting blood glucose level is taken after which they are given a “gluco-cocktail” to drink i.e., a liquid of 100 ccs of glucose. The patient then has their blood glucose level taken hourly for the next four to six hours by the laboratory technician. We also give our patients specific instructions to follow during the time the testing is taking place such as not just sitting in a chair but getting up and moving around to mimic real life. The results are graphed out by the level of blood glucose over the period of time and then interpreted by the practitioner in conjunction with the patient history, physical examination and other lab results. The GTT offers us an accurate view of how the patient’s endocrine, gastrointestinal and nervous systems function in maintaining blood glucose levels under physiological stress i.e., with the car being driven, not just sitting there idling. The amount of practical clinical insights the test provides is often eye opening to the patient and highly useful in setting the patient upon a practical clinical program to reverse chronic disease issues.
In part II of this series on Blood Glucose Regulation, we will explore the Hemoglobin A1C Test and Fasting Insulin Levels and show how integral blood sugar regulation is in reversing chronic disease issues and in preventing chronic disease from starting. We will look at the bodily effects of poorly controlled blood glucose levels including the production of Advanced Glycation End Products and how these interface with autoimmune, cardiovascular, cancer, premature aging, senility and other critical aspects of health.
Case Studies:
Shown below are a few examples of patients from our clinic that successfully reversed their blood sugar issues and regained their health. Note that these patients had other interrelated health issues including digestive issues, cardiovascular issues, thyroid problems, chronic fatigue and obesity.
Case #1: Uncontrolled Diabetes, Cardiovascular Disease, Chronic Fatigue, Obesity
Marji came to the Goldberg Tener Clinic with medical diagnoses of diabetes, high blood pressure, high triglycerides, obesity, depression and chronic fatigue. Her medical physicians prescribed ten different drugs for her to take. In the video interview above, Marji recounts the significant improvement she achieved under our care. Click here to see Marji’s before/after labs which revealed normalization of her blood sugar (hemoglobin A1C) and reduced heart attack / stroke risk (C-Reactive Protein).
Case #2: Diabetes, Severe Diverticulitis, Colitis, Hypertension
Aric had multiple medical diagnoses including diabetes, chronic diverticulitis, colitis, hypertension and obesity. His digestive problems were so severe that his Gastroenterologist advised complete surgical removal of his colon.One year later, Aric is no longer diabetic, his bowel function has normalized with no episodes of diverticulitis, colitis or chronic diarrhea, his blood pressure is normal and, as an additional benefit of getting healthy, he lost 120 pounds. The surgery to remove his colon was cancelled as it was no longer needed. He is drug free. Click here to see Aric’s before/after blood work.
Case #3: Diabetes, Hypertension, Overweight, Hypothyroid, IBS, Drug Induced Liver Injury
Bonnie was diagnosed medically with Type I Diabetes, Hypothyroidism, Hypertension, Irritable Bowel Syndrome, Drug Induced Liver and Kidney Injury and Arthritis. At her initial visit, she was taking a dozen prescription drugs including Atenolol, Amliodipine, Synthroid, Nexium, Benadryl, Limotil, Ventolin and drugs for diabetes including insulin which she had been on for thirteen years. Bonnie is now drug free including being off Insulin and Synthroid which she had been told by her Medical Doctors she would need for life. She lost over 70 pounds and her blood pressure is normal (off drugs). Click here to see Bonny’s before/after blood work.
Definitions:
Blood Glucose – Blood sugar, or glucose, is the primary sugar found in your blood. Your blood carries glucose to all of your body’s cells to use for energy and is controlled primarily by a complex network of glands and their hormones.
Insulin – a hormone produced in the pancreas by the islets of Langerhans, involved in the regulation of of glucose in the blood. A lack of effective insulin is one cause of diabetes.
Insulin Resistance – an impaired response of the body to insulin, resulting in elevated levels of glucose in the blood.
Glycogen- A storage form of glucose.
Glucagon – a hormone formed in the pancreas that helps break down of glycogen to glucose in the liver.
Glycolysis – A process in which glucose (sugar) is partially broken down by cells in enzyme reactions that do not need oxygen.
Gluconeogenesis – the synthesis of glucose from non-carbohydrate sources like lactic acid, glycerol and amino acids occurring in liver and kidneys.
Ketones – a chemical unit your liver produces from fat for energy production when there is not enough carbohydrate/ glucose to supply the body’s fuel needs.
Hypoglycemia – Low blood sugar
Dysglycemia – a condition where the blood glucose goes abnormally high and/ or low and is not being regulated well.




No Comments