05 Mar Successfully Address Allergies

 Paul A. Goldberg MPH, DC, DACBN, DCBCN
Paul A. Goldberg MPH, DC, DACBN, DCBCN
Goldberg Tener Clinic
Chronic Disease Reversal
Over the past decade the Spring Pollens, mostly originating from pollinating trees, have arrived earlier and earlier. This appears due to shifting weather patterns/earlier warm weather. Even just thirty years ago, Spring Pollens would not arrive prior to late February or early March. Now elevated pollen levels are found in mid February. Likewise, Fall pollens are arriving earlier, often starting in mid July not long after the Tree Pollens have subsided. For those with environmental allergies, this often means no respite from suffering.
Our relationship to the world can be divided into two parts; ourselves (self) and everything else that is not us (non-self). To protect ourselves from foreign materials we have an elaborate defense mechanism called the immune system. Twenty-four hours per day, our immune system determines whether anything outside of our own bodies or within our bodies is harmless or represents some degree of danger.
When our immune system determines that any substance e.g., food, pollen, dander, chemical, we have come into contact with is potentially harmful, it gives off chemical messengers for protection. The most well-known chemical is histamine, secreted by white blood cells called mast cells. Histamine causes the mucus membranes including the eyes, mouth, parts of the lung, colon and small intestine to secrete mucus for protection. Under the influence of histamine, the heart speeds up to rid the body of foreign substances and white blood cells increase in number to neutralize the material.
These reactions produce uncomfortable symptoms e.g. sneezing, runny nose, watery eyes, asthmatic attacks and coughing. What few realize, however, is that a variety of other symptoms are also produced in some patients including diarrhea, mucus discharge from the colon, intestinal cramping (as seen in Ulcerative Colitis and Crohn’s Disease) inflammation of the joints as is seen in Rheumatoid Arthritis, eczema, hives, and a myriad of other symptoms. As a chronic disease epidemiologist trained at the University of Texas Medical Center and employed by the State of Illinois in the late 1970’s, I noted that patients with autoimmune disorders such as Rheumatoid Arthritis, Psoriasis, Multiple Sclerosis, Ulcerative Colitis and others, often experienced a crisis with their health during the Spring and Fall when the pollen reached high levels. This association, a causal relationship in my opinion, continues to be largely ignored within medical circles with the prevailing thought that autoimmune disorders are simply “cause unknown”.
Today, many patients relate to us as the Spring Pollination commences, that their autoimmune conditions worsen. Few Medical Allergists understand the relationship between environmental allergies and autoimmune disorders as it has not been part of their medical gospel. Most only acknowledge a limited number of symptoms being related to seasonal allergies e.g. runny nose, watery eyes, sneezing, increased asthma and skin issues. Nonetheless, long experience has demonstrated that seasonal allergies and exacerbations of autoimmune disease are often intimately tied together and that this is a reality and hardship in many patients.
“I Out Grew My Allergies”
It is common to interview patients who relate they had allergies as a child but that they “outgrew them”. Now, however, they are affected by ulcerative colitis, arthritis, ongoing fatigue, headaches and other chronic problems. Their doctors have failed to understand that their allergies were not so much outgrown as they were simply converted into a different set of symptoms.
The medical treatment of allergies involves testing, typically the skin patch test, the “gold standard” in medical offices. This form of testing has been utilized for decades (done on me when I was eleven years old!). In this test, a variety of potential allergens are placed into scratches made on the arm or back to see which ones create a reaction, a reddening of the skin known as an erythema. Then based on the results, allergy (desensitization) shots are administered over a period usually lasting several years, the notion being to accustom the body to the allergen i.e. to desensitize it.
First, recognize that putting a foreign material into a scratch on the skin is not the same as inhaling or ingesting a material. There is, therefore, a high degree of false positives and false negatives with this procedure.
Secondly, desensitization shots entail numerous office visits over a long period of time at considerable expense. All this would be OK if they worked, but a large proportion of patients will tell you that they received little to no benefit from the shots or that their symptoms simply changed to something else or other allergies subsequently developed.
There are also symptomatic allergy treatments both over the counter and prescription. Most involve anti-histamines e.g. Benadryl and Claritin, which block the action of histamine. In more severe cases, corticosteroids are employed which suppress the allergic response and produce a wide range of serious side effects. Steroids will increase the patient’s allergic tendencies over time as the endocrine system is weakened by their use. Steroids also lead to a thinning of the intestinal membrane making the gut more permeable. This allows foreign materials to more easily permeate through the gut lining and initiate an allergic reaction. (See Article: Problems with Prednisone).
Additional Observations
- The number of people in our nation with allergies is dramatically increasing, particularly among children. One of the disorders increasingly seen are the inter-related diseases of Eosinophilic Esophagitis, Gastritis and Colitis which the medical profession treats primarily with steroids. There are many contributing factors to this including children’s lack of exposure to the outside world to develop tolerance to foreign materials and the increased use of pharmaceuticals such as antacids which interfere with proper digestion, particularly of proteins.
- Just as allergies are increasing rapidly so are autoimmune disorders. We consider them to be opposite sides of the same coin. Over the past forty-five years, I have observed the intimate relationship between the two…a relationship important to consider in helping patients improve their health.
- I again emphasize that a wide variety of symptoms, including digestive and intestinal disturbances, fatigue, behavioral issues, depression, respiratory problems and other issues often have allergic components that are overlooked by traditional and alternative medical practitioners.
The Goldberg Bio-Hygienic Re-Creation Approach™
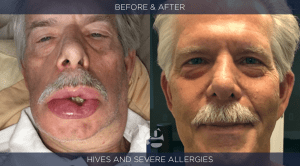


The Goldberg Bio-Hygienic Approach™ focuses on the causal factors behind allergies and autoimmune disorders not their suppression with drugs. Allergy identification is part of the process and we utilize specific testing to evaluate food and inhalant allergies as appropriate. An extensive case history is critical to sort out causal factors. The case history generally takes a full hour and is just as important as laboratory testing. Allergy testing reveals what the patient is currently sensitive to, not why. It should be noted that allergies, particularly to foods, will change over time and that eliminating foods from one’s diet generally only brings about temporary improvement as new allergies typically follow. The why of allergies in each person is more important than just knowing the items they are currently allergic to. We evaluate both.
The immune system interacts intimately with the digestive and endocrine systems. All three deserve attention in allergic issues. Good digestion is critical to overcoming allergies and autoimmune disorders. Dietary factors must be examined but care must be taken not to take an exclusively diet focused approach. Commonly we see patients who have put all their eggs in one basket, in this case the diet basket. More and more foods have often been eliminated till there is little to choose from yet the health problems continue. It is not just the food… it is the way the body processes the food. Carbohydrates must be broken down into glucose, fats into glycerol and fatty acids and proteins into amino acids. If a food is properly digested and broken down into its basic components, allergic reactions are unlikely to occur. Any food mal-digested , however, can set off an allergic response. Foods with a higher protein content and those foods routinely eaten day after day are the most common offenders.
The patient’s endocrine system must be strengthened (unlike the use of steroids by medical physicians which weakens it) so that it is capable of producing the right hormones, in balance with each other, to meet the demands of stress. Blood sugar levels are also important to assess since irregularities in blood glucose can exacerbate allergic tendencies.
Rest and sleep habits must be assessed whereas a tired individual is much more likely to have more severe allergic problems.
Emotional stressors must be evaluated as emotional ups and downs are significant factors in the exacerbation of allergic problems.
In sum, the Bio-Hygienic Approach™, rather than treat allergies, seeks out the causal factors behind them and then creates the right conditions to foster a more balanced, healthy response to the outside world whether the instigating factors be foods, pollens, dander or other foreign materials.
The outcome through such an approach is improved overall health and fewer, less severe, allergic responses without the use of dangerous drugs. As with any chronic health issue, there is the need for proper evaluation followed by discipline in enacting a full health building program individualized to the patient.
Click here to see case studies exemplifying the Goldberg Bio-Hygienic Approach in action.
Related Articles
- Eosinophilic Esophagitis, Gastritis and Colitis
- Reversing Autoimmune Disease
- Problems with Prednisone: Why Inflammation is Not the Enemy
- Crohn’s Disease and Ulcerative Colitis: Your Health Can be Restored!
- An Effective Causal Based Approach to Digestive Disorders
- Skin Deep: A Closer Look at Dermatological Issues




No Comments